Normal Anatomy of the Knee Joint
How does the Knee joint work?
The knee joint, which appears like a simple hinge-joint, is one of the most complex joint. It consists of the femur (thighbone), tibia (shinbone) and patella (kneecap). Knee Anatomy The knee is a synovial joint, which means it is lined by synovium. The synovium produces fluid lubricating and nourishing the inside of the joint. Articular cartilage is the smooth surfaces at the end of the femur and tibia. It is the damage to this surface, which causes arthritis.Skeletal Anatomy
Femur
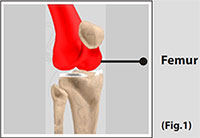
Femur The femur (thighbone) is the largest and the strongest bone in the body. It is the weight-bearing bone of the thigh. It provides attachment to most of the muscles of the knee.
(Refer fig. 1)
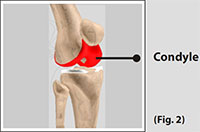
Condyle
The two femoral condyles make up for the rounded end of femur. Its smooth articular surface allows the femur to move easily over the tibial (shinbone) meniscus.
(Refer fig. 2)
Tibia
The tibia (shinbone) the second largest bone in the body is the weight bearing bone of the leg. The menisci incompletely cover the superior surface of the tibia where it articulates with the femur. The menisci act as shock absorbers, protecting the articular surface of the tibia as well as assisting in rotation of the knee. (Refer fig. 3)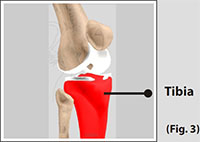
Fibula
The fibula, although not a weight bearing bone, provides attachment sites for the Lateral Collateral Ligaments (LCL) and the biceps femoris tendon. The articulation of tibia and fibula, also allows a slight degree of movement, providing an element of flexibility in response to the actions of muscles attaching to the fibula. (Refer fig. 4)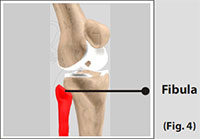
Patella
The Patella (kneecap), attached to the quadriceps tendon above and the patellar ligament below, rests against the anterior articular surface of the lower end of the femur and protects the knee joint. The patella acts as a fulcrum for the quadriceps by holding the quadriceps tendon off the lower end of the femur. (Refer fig. 5)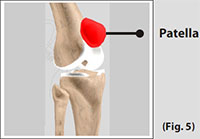
Menisci
The medial and the lateral meniscus are thin C-shaped layers of fibrocartilage, incompletely covering the surface of the tibia where it articulates with the femur. The majority of the meniscus has no blood supply and for that reason, when damaged the meniscus is unable to undergo the normal healing process that occurs in the rest of the body. In addition, meniscus begins to deteriorate with age, often developing degenerative tears. Typically, when the meniscus is damaged, the torn pieces begin to move in an abnormal fashion inside the joint. The menisci act as shock absorbers, protecting the articular surface of the tibia as well as assisting in rotation of the knee. As secondary stabilizers, the intact menisci interact with the stabilizing function of the ligaments and are most effective when the surrounding ligaments are intact. (Refer fig. 6)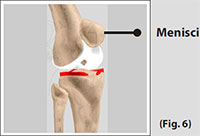
Soft Tissue Anatomy
Anterior Cruciate Ligament (ACL)
The anterior cruciate ligament (ACL) is the major stabilizing ligament of the knee. The ACL is located in the center of the knee joint and runs from the femur (thigh bone) to the tibia (shin bone), through the center of the knee. The ACL prevents the femur from sliding backwards on the tibia (or the tibia sliding forwards on the femur). Together with Posterior Cruciate Ligament (PCL). ACL stabilizes the knee in a rotational fashion. Thus, if one of these ligaments is significantly damaged, the knee will be unstable when planting the foot of the injured extremity and pivoting, causing the knee to buckle and give way.
(Refer fig. 7)

Posterior Cruciate Ligament (PCL)
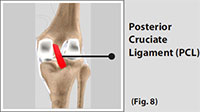
Much less research has been done on the posterior cruciate ligament (PCL) because it is injured far less often than the ACL. The PCL prevents the femur from moving too far forward over the tibia. The PCL is the knee’s basic stabilizer and is almost twice as strong as the ACL. It provides a central axis about which the knee rotates.
(Refer fig. 8)
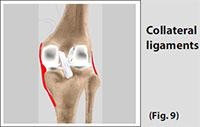
Collateral Ligaments
Collateral Ligaments prevent hyperextension, adduction, and abduction.
- Superficial MCL (Medial Collateral Ligament) connects the medial (inner) epicondyle of the femur to the medial condyle of the tibia and resists valgus (bending out) force.
- Deep MCL (Medial Collateral Ligament) connects the medial (inner) epicondyle of the femur with the medial meniscus.
- LCL (Lateral Collateral Ligament), entirely separate from the articular capsule, connects the lateral (outer) epicondyle of the femur to the head of the fibula and resists varus (bending in) force.
(Refer fig. 9)
Biomechanics of the Knee
Flexion
When the knee is flexed or bent, the cruciate ligament is taut and the collateral ligaments are relaxed. Maximum flexion of the knee is 120-150 degrees. (Refer fig. 10)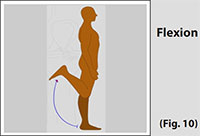
Extension
When the knee is extended or straightened, the lateral and medial collateral ligaments as well as the ACL are taut. Maximum extension of the knee is 5-10 degrees. (Refer fig. 11)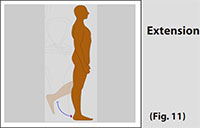
Medial Rotation
This movement can only be achieved while the knee is in flexion. The cruciate ligaments control medial rotation of the tibia by twisting around each other to enable this movement. Maximum internal rotation is 30-40 degrees. (Refer fig. 12)
Lateral Rotation
This movement also requires the knee to be flexed in order to rotate laterally. The cruciate ligaments control lateral rotation of the tibia by untwisting around each other to enable this movement. Maximum external rotation is 30-40 degrees. (Refer fig. 13)
